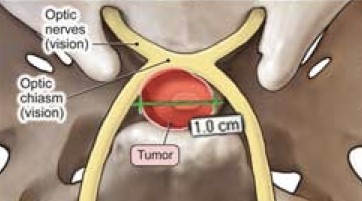
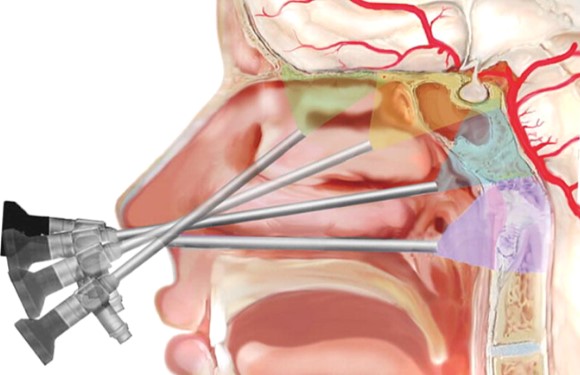
Pituitary gland is situated in the centre of the head below the brain, behind the eyes and above the back of the nose. It controls other endocrine glands – Thyroid, adrenal glands, ovaries, breast in women and testes in men. It also secretes growth hormone and anti-diuretic hormone.
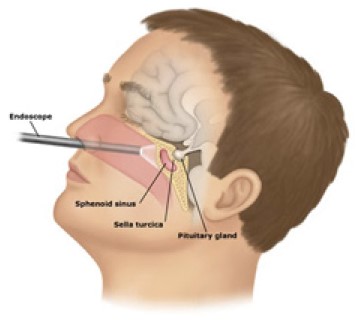
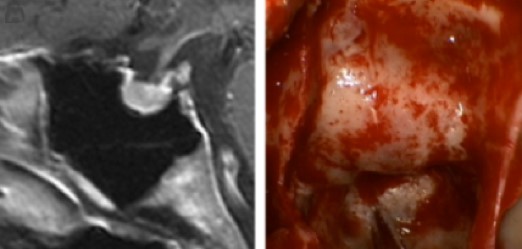
A tumor from this gland may secrete hormones excessively (even when <10mm, called Microadenoma) causing conditions like Acromegaly, Cushing’s disease, or infertility-related syndromes. Non-functioning tumors can grow and compress nearby structures, leading to vision problems or hormone deficiency. Many are detected incidentally during scans.